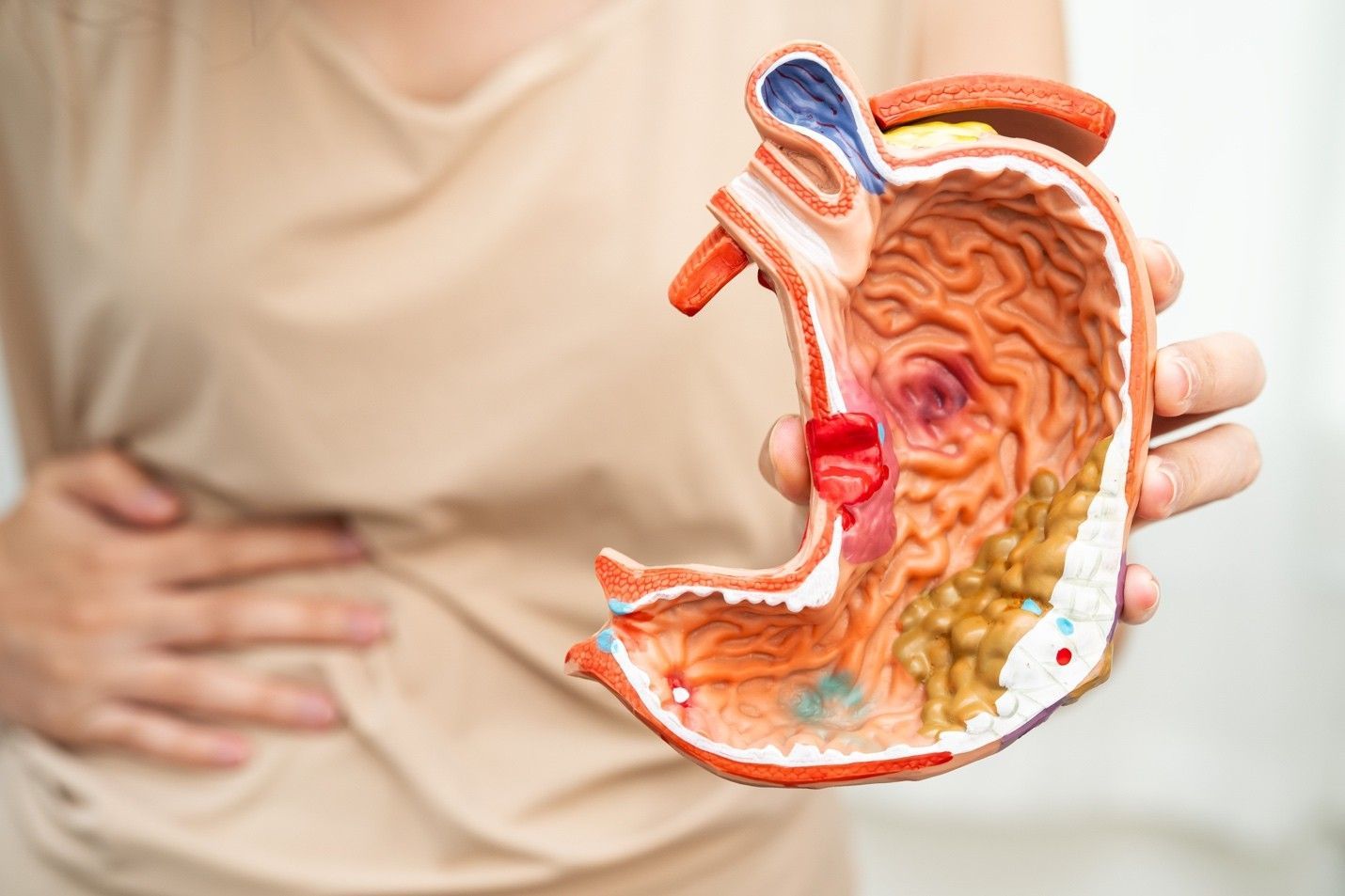
Tests to Detect and Treat Esophageal Disorders

The esophagus is a muscular tube that connects the throat to the stomach. Its primary function is to transport food and liquids from the mouth to the stomach for digestion. However, this crucial organ is also prone to various disorders that can affect its ability to function properly.
What Are Esophageal Disorders?
Esophageal disorders refer to any medical condition that affects the esophagus. These conditions can range from mild to severe and can cause a wide range of symptoms such as heartburn, difficulty swallowing, regurgitation, and chest pain. Some of the most common esophageal disorders include gastroesophageal reflux disease (GERD), Barrett's esophagus, esophageal cancer, achalasia, and eosinophilic esophagitis.
The prevalence of esophageal disorders is high, and the incidence of these conditions has been increasing over the past few decades. According to recent
studies, GERD alone affects up to 27% of the adult population in the United States, making it one of the most common digestive disorders. Esophageal cancer is also one of the fastest-growing cancers in the country, with more than 18,000 new cases diagnosed each year.
Early detection and treatment of esophageal disorders is essential to prevent further complications and improve patient outcomes. Delayed diagnosis and treatment can lead to severe complications such as bleeding, ulcers, and even cancer. Therefore, it is crucial to seek medical attention if you experience any symptoms related to esophageal disorders.
What Are Some Common Esophageal Disorders?
Esophageal disorders are diverse, and each one of them presents unique symptoms and challenges. Here are some of the most common types of esophageal disorders.
Gastroesophageal Reflux Disease (GERD)
GERD is a chronic digestive disorder that occurs when stomach acid flows back into the esophagus, causing irritation and inflammation. This condition can cause symptoms such as heartburn, chest pain, regurgitation, and difficulty swallowing. Long-term untreated GERD can lead to complications such as esophageal ulcers, bleeding, and even cancer.
Treatment options for GERD include lifestyle changes such as dietary modifications, weight loss, and quitting smoking. Medications and surgery may be required in other cases, based on severity.
Barrett's Esophagus
Barrett's esophagus is a condition that results from chronic GERD. In this condition, the lining of the esophagus changes to resemble the lining of the intestine, increasing the risk of developing esophageal cancer. Patients with Barrett's esophagus are typically monitored closely for signs of cancer, and treatment options may include endoscopic procedures to remove abnormal tissue or surgery to remove the affected part of the esophagus.
Esophageal Cancer
Esophageal cancer is a rare but deadly form of cancer that typically affects older adults. The most common types of esophageal cancer are adenocarcinoma and squamous cell carcinoma. Symptoms of esophageal cancer can include difficulty swallowing, unintentional weight loss, chest pain, and a persistent cough. The most common treatment options for esophageal cancer are surgery, chemotherapy, and radiation therapy.
Achalasia
Achalasia is a rare disorder that affects the muscles in the esophagus, making it difficult for food and liquid to pass through to the stomach. Symptoms of achalasia can include difficulty swallowing, regurgitation, chest pain, and heartburn. Achalasia can be treated with medications, endoscopic procedures to stretch the esophagus, or surgery to remove the affected portion of the esophagus.
Eosinophilic Esophagitis
Eosinophilic esophagitis is a condition in which the esophagus becomes inflamed due to an allergic reaction to certain foods or environmental triggers. Symptoms of eosinophilic esophagitis can include difficulty swallowing, chest pain, and food impaction. Treatment options for eosinophilic esophagitis include dietary changes, medications, or endoscopic procedures to remove any obstructing food.
Early diagnosis and treatment are essential to managing these conditions and improving patient outcomes. If you experience any symptoms related to esophageal disorders, it's important to seek medical attention promptly.
What Diagnostic Tests Can Be Used to Diagnose Esophageal Disorders?
The diagnosis of esophageal disorders usually involves a combination of patient history, physical examination, and diagnostic tests. Here are some of the most common diagnostic tests for esophageal disorders.
Esophagogastroduodenoscopy (EGD)
EGD is a diagnostic procedure in which a flexible tube with a light and camera is inserted through the mouth into the esophagus, stomach, and duodenum. This test allows the doctor to visually examine the lining of the esophagus and stomach for any abnormalities such as inflammation, ulcers, or tumors. EGD can also be used to take tissue samples (biopsies) for further analysis. EGD is typically performed under sedation and takes about 15-30 minutes.
Barium Swallow Test
A barium swallow test is a diagnostic imaging test that involves swallowing a liquid containing barium, a contrast material that shows up on X-rays. This test allows the doctor to visualize the esophagus as the barium passes through it, highlighting any abnormalities such as strictures (narrowing) or diverticula (outpouching). The test can be performed either as a single X-ray or as a series of X-rays taken at various intervals.
pH Monitoring
PH monitoring is a diagnostic test that measures the acidity (pH) in the esophagus over a period of time. This test is typically used to diagnose GERD, as it can detect abnormal acid reflux even when patients don't have symptoms. pH monitoring can be done in several ways, including placing a small tube through the nose into the esophagus or using a wireless pH monitoring device that is temporarily attached to the esophagus. The test usually takes 24 to 48 hours and allows doctors to assess the frequency and severity of acid reflux episodes.
High-Resolution Manometry
High-resolution manometry is a diagnostic test that evaluates the function of the esophageal muscles and how they contract to move food and liquids into the stomach. This test uses a thin, flexible tube with sensors to measure pressure changes in the esophagus as the patient swallows. High-resolution manometry can detect esophageal motility disorders such as achalasia, as well as other conditions that affect the normal function of the esophagus. Usually, this test takes 30 minutes and is performed under sedation.
Endoscopic Ultrasound (EUS)
Endoscopic ultrasound (EUS) is a diagnostic procedure that combines an endoscope (a flexible tube with a light and camera) and ultrasound technology. EUS allows doctors to visualize and evaluate the layers of the esophagus and surrounding tissues in high detail. This test can be used to diagnose esophageal cancer and other conditions that affect the esophagus, such as Barrett's esophagus. EUS can also be used to guide biopsies and other therapeutic procedures. Generally, EUS takes about 30 to 60 minutes to perform under sedation.
To sum it up, there are several diagnostic tests available for the evaluation of esophageal disorders.
Esophagogastroduodenoscopy
(EGD) is the gold standard for visualizing the esophagus and taking biopsies. pH monitoring and high-resolution manometry can help diagnose motility disorders and GERD. Endoscopic ultrasound (EUS) provides detailed imaging of the esophageal wall and surrounding tissues and is useful for diagnosing esophageal cancer and other conditions. Your healthcare provider can help determine which diagnostic test is right for you based on your symptoms and medical history.
The treatment of esophageal disorders depends on the specific condition and severity of the disease. Read on for a gist of some of the most common treatment options.
Treatment Options for Esophageal Disorders
Lifestyle Changes
In many cases, lifestyle modifications can help manage esophageal disorders. These modifications may include dietary changes, such as avoiding spicy or acidic foods and consuming smaller, more frequent meals. Weight loss and smoking cessation are also recommended, as excess weight and smoking can exacerbate esophageal disorders.
Medications
Medications are commonly used to manage the symptoms of esophageal disorders. Proton pump inhibitors (PPIs) are frequently prescribed for gastroesophageal reflux disease (GERD) and work by reducing the amount of acid produced by the stomach. Antacids can also provide relief by neutralizing stomach acid. Muscle relaxants may be prescribed for esophageal motility disorders to help the muscles in the esophagus relax and move food more easily.
Surgical Interventions
In some cases, surgery may be necessary to treat esophageal disorders. Fundoplication is a common surgical procedure used to treat GERD. The procedure involves wrapping the upper part of the stomach around the lower part of the esophagus to create a barrier against reflux. Esophagectomy is another surgical option for esophageal cancer or severe GERD. This procedure involves removing part or all of the esophagus and reconstructing it using other tissue.
Endoscopic Therapies
Endoscopic therapies involve using an endoscope to deliver treatment directly to the esophagus. Radiofrequency ablation (RFA) is a minimally invasive treatment option that uses high-frequency energy to remove diseased tissue in the esophagus. It is an effective treatment for certain esophageal disorders, such as Barrett's esophagus and early-stage esophageal cancer.
During the procedure, a catheter is inserted into the esophagus and delivers controlled energy to the affected area, causing the removal of diseased tissue. RFA has a high success rate and a low risk of complications, making it a viable option for many patients with esophageal disorders.
At
Northlake Gastroenterology Associates, our team of experienced gastroenterologists is dedicated to providing personalized care for patients with esophageal disorders. We offer a
range of diagnostic tests and treatment options to help manage your condition and improve your quality of life.
If you or a loved one is experiencing symptoms of an esophageal disorder, we encourage you to
request an appointment.
Our team can help determine the underlying cause of your symptoms and develop a customized treatment plan to meet your needs.
More Blogs