Tips for Managing Diverticulitis

What is Diverticulitis?
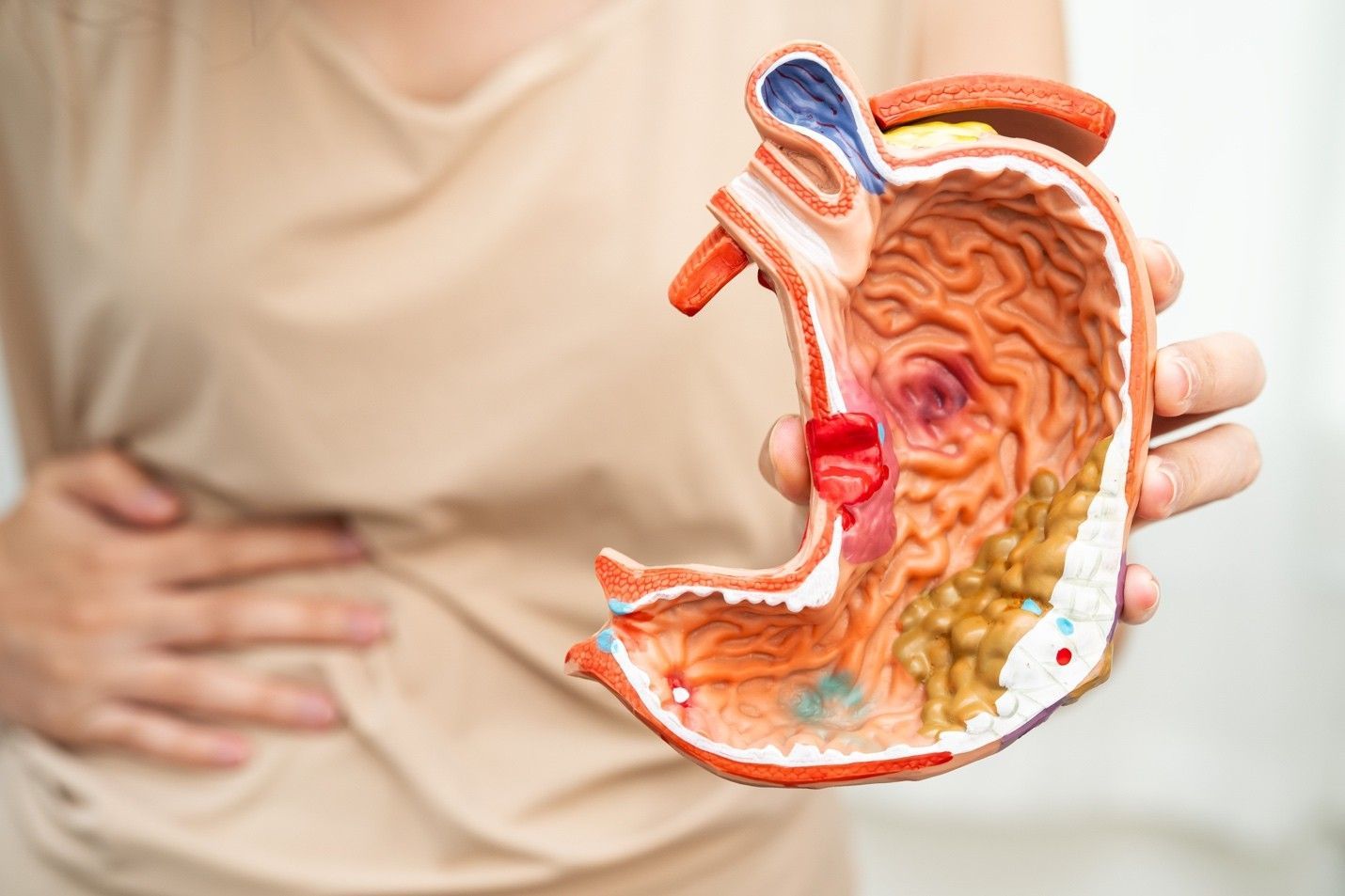
Diverticulitis is a condition that occurs when small pockets or sacs, known as diverticula, form in the lining of the colon and become inflamed or infected. Diverticula are common in the large intestine or colon, especially as people age. However, not all individuals with diverticula will experience diverticulitis.
When a diverticulum becomes inflamed or infected, it can cause a range of
uncomfortable symptoms. In some cases, diverticulitis can lead to complications such as abscesses, perforation of the colon, and fistulas.
The exact cause of diverticulitis is unknown, but it is believed to be related to a combination of factors such as a diet low in fiber, obesity, aging, genetics, and a sedentary lifestyle.
Tips to Manage for Diverticulitis
The treatment for diverticulitis depends on the severity of the condition. Mild cases of diverticulitis can be treated with simple tips, while severe cases may require hospitalization and intravenous antibiotics. The treatment options include:
Dietary Changes
Following a high-fiber diet is an essential part of managing diverticulitis. A high-fiber diet helps promote regular bowel movements, prevent constipation, and reduce inflammation in the colon. Here are some tips for incorporating more fiber into your diet:
Eat Plenty of Fruits and Vegetables
These are excellent sources of fiber and should be included in your diet every day. Try to choose a variety of colorful fruits and vegetables to get a range of nutrients.
Choose Whole Grains
Instead of refined grains, choose whole-grain bread, pasta, and rice, which are high in fiber. Look for products that list "whole grain" as the first ingredient.
Add Legumes
Beans, lentils, and peas are excellent sources of fiber and can be added to soups, salads, or casseroles.
Snack on Nuts and Seeds
Almonds, sunflower seeds, and pumpkin seeds are all high in fiber and make a great snack.
Drink Plenty of Water
As you increase your fiber intake, it is important to drink plenty of water to prevent constipation and ensure the fiber moves smoothly through your digestive system.
It is important to increase your fiber intake gradually to avoid bloating, gas, and other digestive symptoms. Aim for at least 25-30 grams of fiber per day, and consider working with a registered dietitian to develop a personalized diet plan that meets your needs.
Exercise Regularly
Regular exercise is an important aspect of managing diverticulitis. Exercise can help promote regular bowel movements, reduce inflammation in the colon, and improve overall health and well-being. Here are some tips for incorporating exercise into your routine:
Start Slow
If you are new to exercise, start slowly and gradually increase the intensity and duration of your workouts. Walking is an excellent form of low-impact exercise that is easy to start and can be done almost anywhere. This can include activities such as brisk walking, cycling, swimming, or dancing. If you are unable to do 30 minutes at a time, try breaking it up into shorter sessions throughout the day.
Include Strength Training
Strength training can help improve muscle tone and reduce the risk of falls and fractures. Use free weights, resistance bands, or bodyweight exercises to work all major muscle groups.
Listen to Your Body
If you experience pain or discomfort during exercise, slow down or stop and rest. It is important to talk to your healthcare provider before starting a new exercise program, especially if you have any medical conditions or injuries. Make exercise a regular part of your routine, and try to find activities that you enjoy to help keep you motivated.
Know the Signs and Symptoms of a Flare-up
Knowing the signs and symptoms of a diverticulitis flare-up is important for managing the condition and preventing complications. Here are some common symptoms to watch for:
Abdominal Pain
The most common symptom of diverticulitis is abdominal pain, which is often felt on the left side of the abdomen. The pain may be severe and persistent, and may worsen with movement or when the affected area is touched.
Nausea and Vomiting
These symptoms may occur along with abdominal pain and can be a sign of an infection or inflammation in the colon.
Changes in Bowel Movements
During an acute episode of diverticulitis, it may be recommended to avoid solid foods and switch to a liquid diet or a low-fiber diet for a short period of time. This will allow the colon to rest and heal.
Rectal Bleeding
In some cases, diverticulitis can cause rectal bleeding, which may appear as bright red blood in the stool or on toilet paper.
Surgery
Surgery is not always necessary for diverticulitis. But in some cases, it may be recommended by your healthcare provider. Here are some reasons why surgery may be necessary:
Recurrent or Severe Attacks
If you have recurrent or severe episodes of diverticulitis that do not respond to other treatments, surgery may be recommended.
Complications
If you develop complications such as a perforation or abscess in the colon, surgery may be necessary to remove the affected portion of the colon.
Chronic Diverticulitis
In some cases, diverticulitis can become chronic and cause ongoing symptoms. Surgery may be recommended in these cases to remove the affected portion of the colon.
Types of Surgery for Diverticulitis
In this topic, we will explore the different types of surgical treatment options for diverticulitis in more detail.
Laparoscopic Surgery
Laparoscopic surgery, also known as minimally-invasive surgery or keyhole surgery, is a type of surgery for diverticulitis that involves making several small incisions in the abdomen instead of a large incision. This approach uses a laparoscope, which is a thin, flexible tube with a camera and light attached to it, to provide a view of the inside of the abdomen on a monitor.
During laparoscopic surgery for diverticulitis, the surgeon makes several small incisions in the abdomen and inserts the laparoscope and other specialized instruments through these incisions. The surgeon then uses these instruments to remove the affected portion of the colon and repair or reconnect the remaining portions of the colon. In some cases, a temporary colostomy may be necessary if the affected portion of the colon cannot be reconnected.
Colon Resection
Colon resection is a surgical procedure that involves removing a portion of the colon or large intestine. This procedure may be recommended for a variety of reasons, including diverticulitis, colorectal cancer, inflammatory bowel disease, and other conditions that affect the colon.
During a colon resection, the surgeon makes an incision in the abdomen and removes the affected portion of the colon. The remaining portions of the colon are then reconnected, either through a primary anastomosis (reconnecting the two ends of the colon) or through a colostomy (creating an opening in the abdomen to allow waste to be eliminated from the body).
Loop Ileostomy
A loop ileostomy is a surgical procedure in which a loop of the small intestine (the ileum) is brought to the surface of the abdomen through an opening called a stoma. This procedure is typically done as a temporary measure to divert stool away from a section of the bowel that needs time to heal or recover.
During a loop ileostomy procedure, the surgeon makes an incision in the abdomen and brings a loop of the ileum to the surface. The loop is then divided, with one end being attached to the skin to form the stoma, and the other end being left attached to the remaining intestine. Stool is diverted through the stoma and collected in a pouch worn on the outside of the body.
Laparoscopic Washout
Laparoscopic washout is a surgical procedure used to treat acute diverticulitis. It involves using a laparoscope to visualize and clean out the infected or inflamed area of the colon.
During a laparoscopic washout, the surgeon makes several small incisions in the abdomen and inserts the laparoscope and other surgical instruments. The surgeon then irrigates the infected area with a sterile saline solution to wash out any pus or debris. The colon is inspected to ensure that there are no perforations or other complications. Any damaged tissue or abscesses will be removed.
The benefits of laparoscopic washout over traditional open surgery for acute diverticulitis include less pain, shorter hospital stay, and faster recovery time. However, it may not be appropriate for all patients and is typically only recommended for those with mild to moderate diverticulitis who do not have significant complications.
Managing diverticulitis can be challenging, but with the right tools and guidance, it is possible to live a comfortable and healthy life. At
Northlake Gastroenterology, we are dedicated to providing high-quality care and personalized treatment plans for our patients with diverticulitis. If you or a loved one are experiencing symptoms of diverticulitis or have questions about managing the condition, please contact us today to
schedule an appointment
with one of our experienced gastroenterologists.
More Blogs